Dedicated caregivers in long term care facilities across the country continue to do everything possible to protect their residents. But as nursing homes and assisted living communities have invested in the resources needed to keep their residents and staff safe, the financial impact on providers has grown. Already some facilities have been forced to close, and more could soon follow if lawmakers don’t act.
The long term care sector has long faced financial struggles, but the pandemic has exacerbated these severe challenges. Medicaid is the primary payer for nursing homes, covering more than 60 percent of all nursing home residents and approximately 50 percent of costs for all long term care services. However, Medicaid reimbursements only cover 70 to 80 percent of the actual cost of nursing home care. This chronic gap in funding has resulted in shoestring budgets and ongoing operating losses for nursing home providers.
Coupled with the current need to acquire more personal protective equipment (PPE), regular COVID testing and staffing needs associated with the pandemic, these facilities are being pushed to the brink of closure. Already, facilities in
California,
Colorado,
Michigan,
New Hampshire,
New York and
Rhode Island have announced permanent closures or have warned that closures are looming.
A nursing home in Pennsylvania also recently
announced that the facility will be closing in January because of financial difficulties. The Charles Morris Nursing Home cited the increased cost of care during the pandemic combined with low Medicaid reimbursement rates as the cause for the closure. As
The New York Times highlighted last year, facility closures will hit rural communities especially hard has families will be left with few options for the care of their loved ones.
The American Health Care Association and National Center for Assisted Living (AHCA/NCAL) conducted a
survey that found that more than half of nursing homes are currently operating at a loss and 72 percent of operators say they won’t be able to sustain operation another year at the current pace.
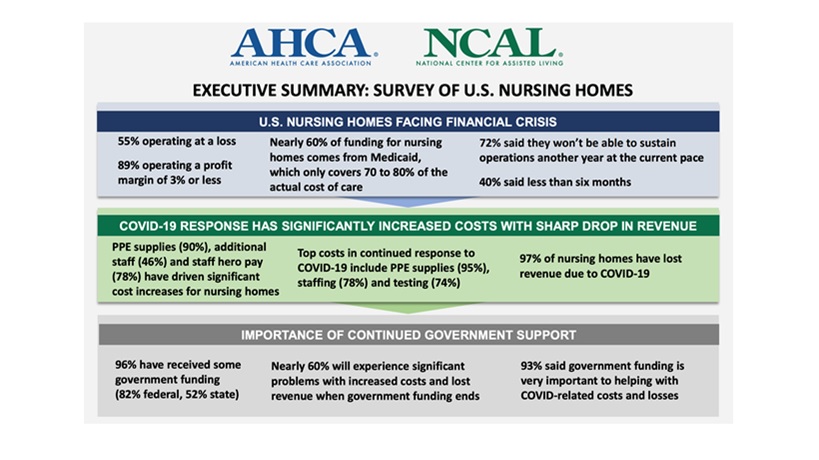
Nursing homes and assisted living communities across the country face the same fate as Charles Morris Nursing Home if more is not done to support the long term care sector. Congressional funding is needed to help facilities combat the ongoing pandemic, but long term solutions are also called for, such as higher Medicaid reimbursements rates that reflect the actual cost of care so nursing homes and assisted living communities no longer have to face these financial difficulties. Abruptly moving elderly patients out of their communities and forcing them to find new care takes a heavy toll. We must ensure every facility has the means to provide the highest quality of care for our most vulnerable population.
ABOUT AHCA/NCAL
The American Health Care Association and National Center for Assisted Living (AHCA/NCAL) represents more than 14,000 non-profit and proprietary skilled nursing centers, assisted living communities, sub-acute centers and homes for individuals with intellectual and development disabilities. By delivering solutions for quality care, AHCA/NCAL aims to improve the lives of the millions of frail, elderly and individuals with disabilities who receive long term or post-acute care in our member facilities each day. For more information, please visit
www.ahcancal.org or
www.ncal.org.